-

Hear from Professor Monica Toft
Learn how Professor Monica Toft is shaping the study of global affairs and diplomacy at Fletcher.
Hear from Prof. Toft -

Explore Fletcher academics in action
Fletcher Features offers insights, innovation, stories and expertise by scholars.
Get global insights -
Get application tips right from the source
Learn tips, tricks, and behind-the-scenes insights on applying to Fletcher from our admissions counselors.
Hear from Admissions -

Research that the world is talking about
Stay up to date on the latest research, innovation, and thought leadership from our newsroom.
Stay informed -
Meet Fletcherites and their stories
Get to know our vibrant community through news stories highlighting faculty, students, and alumni.
Meet Fletcherites -

Forge your future after Fletcher
Watch to see how Fletcher prepares global thinkers for success across industries.
See the impact -

Global insights and expertise, on demand.
Need a global affairs expert for a timely and insightful take? Fletcher faculty are available for media inquiries.
Get in Touch
Unlocking Value through Virtualized Healthcare: Which Countries are Ready?
Digital Planet analyzes and benchmarks 46 countries on their measures of digitalization and healthcare capacities, revealing "sweet spots" for virtual healthcare across the globe.
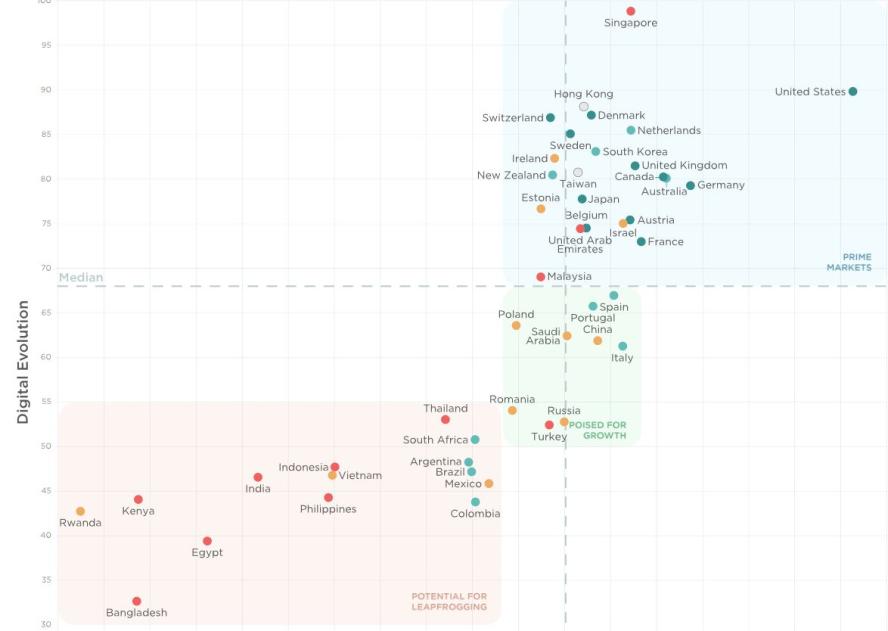
The state of digitization of healthcare delivery globally is quite uneven, spotted with patches of excellence and falling well short in others. Digitally administered medicine is yet to reach corners of the world where its need is the greatest. Our study spanning 46 countries, where we overlaid our measures of digitalization and healthcare capacity, reveals sweet spots for virtualized healthcare and how countries lagging in critical healthcare infrastructure can leapfrog by deploying digital mechanisms to provide quality healthcare to their masses.
The health care industry globally has a reputation for being slow to digitization compared to other consumer industries such as travel, retail, and financial services. While these industries are not all regulated alike and the healthcare industry is, for good reasons, more heavily regulated and is expected – much more than others – to thread the needle between “first, do no harm” and “moving fast” without breaking things, such perceptions of low and slow adoption of digital technologies have some basis in fact. The consumer-facing and primary care aspects of the industry have certainly been slower to digitization; case in point: the reams of paperwork filled out by patients at clinics on a daily basis in most parts of the world and the ubiquity of fax machines across the American medical sector to this date, three decades after most other industries jettisoned them.
And yet, technological innovations and innovation enabling policies, have been permeating various facets of healthcare delivery around the world. These innovations and policies are widely distributed across the care delivery system writ large – sometimes tangible, other times barely visible – such as regulations governing cross-border flows of healthcare data, digitally intermediated real-time critical care across time zones, and the electronic identity enabled system-wide digitization of healthcare delivery. Consider advanced economies such as Estonia where 99% of all health data and prescriptions are digitized as is the entire billing process, all of which runs on the rails of a digital identity-based nationwide electronic health record network, and New Zealand, where the government instituted a citizen privacy preserving “we will ask only once” policy approach to digital public services such as verifiable claims including all aspects of healthcare. Innovations, albeit of a frugal variety, have taken root in the global south despite (or perhaps because of) capacity constraints in digital connectivity and healthcare infrastructure. Consider Ziqitza Health Care Limited, a social enterprise that provides ambulance services to all segments of society in several parts of India using basic call center infrastructure.
Within the care delivery value chain, there are spots of digital distinction in secondary and tertiary care. Consider the recent pioneering partnership between Emory Healthcare, Royal Perth Hospital in Australia, and Philips, a technology company, which is pushing the frontiers of digital globalization of critical care by facilitating Emory ICU physicians and nurses to deliver real-time care “from the other side of the Earth by working in daylight hours in Australia to cover nighttime hours in Atlanta.” In recent years, digital health-focused startups have been active in many parts of the world across several functions of care delivery: from administrative automation, clinical intelligence, and pharma supply chains to virtual care delivery, drug discovery, and screening and diagnostics.
All innovations considered, the state of digitization of healthcare delivery globally is quite uneven — spotted with patches of excellence and falling well short in others. Digitally administered medicine is yet to reach corners of the world where its need is the greatest.
The pandemic has both exposed this state of unevenness around the world and accelerated the embrace of digital technologies by healthcare providers and patients alike especially in the delivery of primary care. Telemedicine, online pharmacies, online therapy and wellness, and the use of wearable monitoring devices have been on the rise through 2020. Consumers and providers are warming up to the value potential of telemedicine and virtualized medicine. In a recent survey of consumers in the United States, convenience, speed, and quality care were rated among the top reasons for using telehealth services. A study by McKinsey & Company, a consultancy, noted that a sustained acceleration of the pandemic-induced trends of consumer and provider adoption of telehealth and the extension of telemedicine beyond virtual urgent care into virtualizing other aspects of healthcare delivery in the United States could unlock value to the tune of “approximately US$250 billion or ~20% of all Medicare, Medicaid, and commercial outpatient, office, and home health spend.”
With a view to providing guidance to policymakers, decisionmakers, technologists and healthcare administrators, we posed the question, which countries are most ready to unlock value though delivery of virtualized healthcare at scale?

